Because online forms often collect patient health information. Once that happens, HIPAA applies, and the data needs to be protected the same way it would be inside a medical system.
What Happens If Forms Aren’t HIPAA Compliant? (2026)
Learn what happens when forms aren’t HIPAA compliant, data breaches, penalties, and trust loss. A simple 2026 guide to risks and prevention.

HIPAA non-compliance creates risk that compounds risk and criminal charges, quickly.
HIPAA, the Health Insurance Portability and Accountability Act, is a U.S. law designed to protect patient health information. It sets clear guidelines for how healthcare data should be collected, stored, and shared, including data collected through online forms.
When forms aren’t HIPAA compliant, the consequences are real and often serious. Patient data can be exposed, organizations can face compliance violations, and trust can be lost with very little warning. What starts as a small oversight, such as using the wrong form tool or template, can quickly turn into a breach investigation, regulatory scrutiny, or reputational damage that’s difficult to undo.
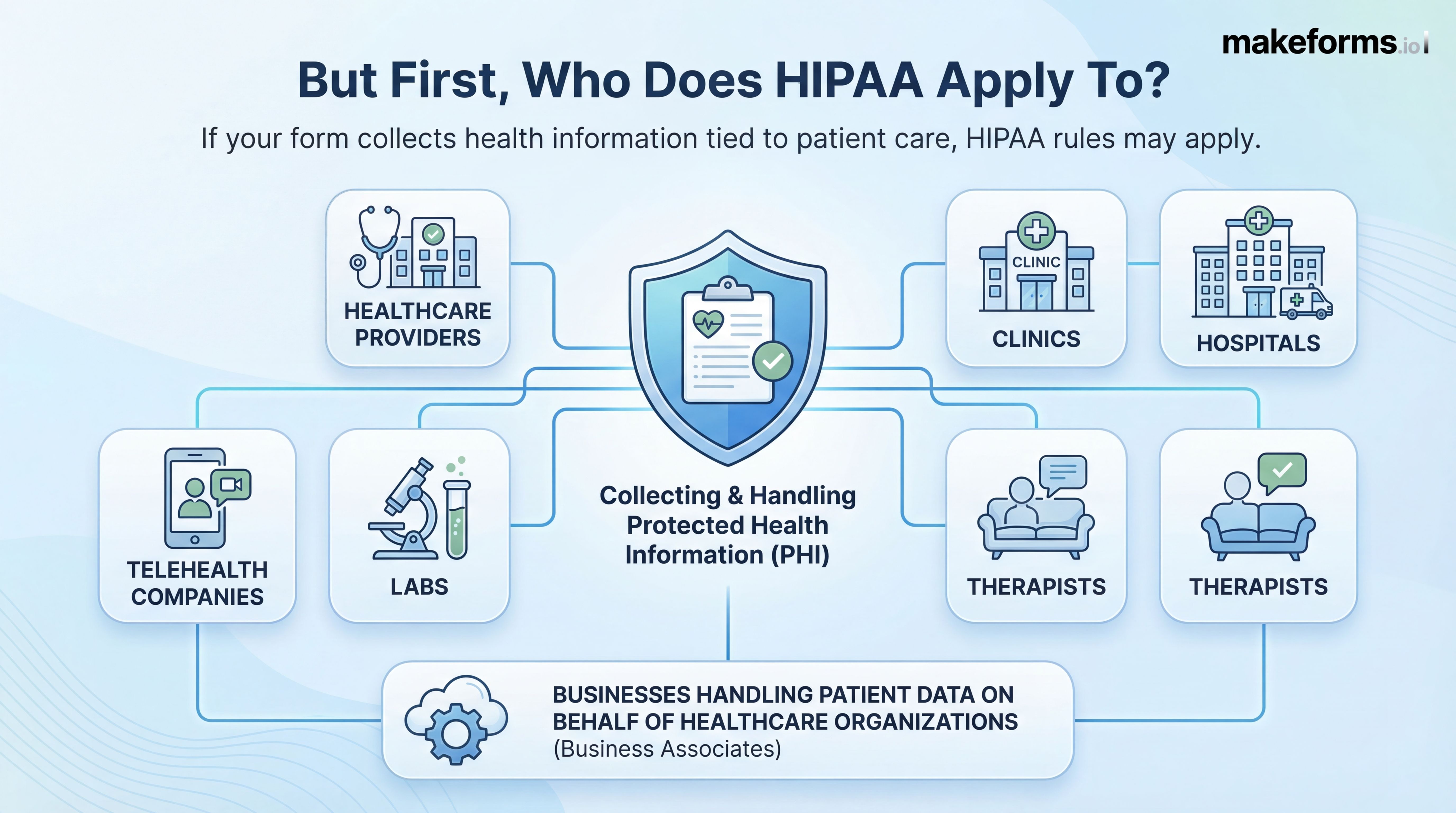
But First, Who Does HIPAA Apply to?
HIPAA applies to covered entities, including healthcare providers, clinics, hospitals, therapists, labs, telehealth companies, and businesses that handle patient data on their behalf. If your online forms collect health details, symptoms, or information connected to patient care, HIPAA rules apply, even if the form is used only occasionally or for a single workflow.
The challenge is that these risks aren’t always obvious upfront. Familiar form tools, basic templates, or searches for “hippa forms” can feel safe, especially when the form works and nothing appears broken. But HIPAA compliance depends on how data is handled behind the scenes, not just how a form looks.
This guide explains what HIPAA compliance means for online forms, what can go wrong when forms aren’t set up correctly, and how to avoid issues that can grow quickly and become costly in 2026.
What you can takeaway from this article
- What are the real consequences when HIPAA compliance is violated (including breach scenarios)
- What to look for in HIPAA compliant forms so compliance is built into the workflow, not added later
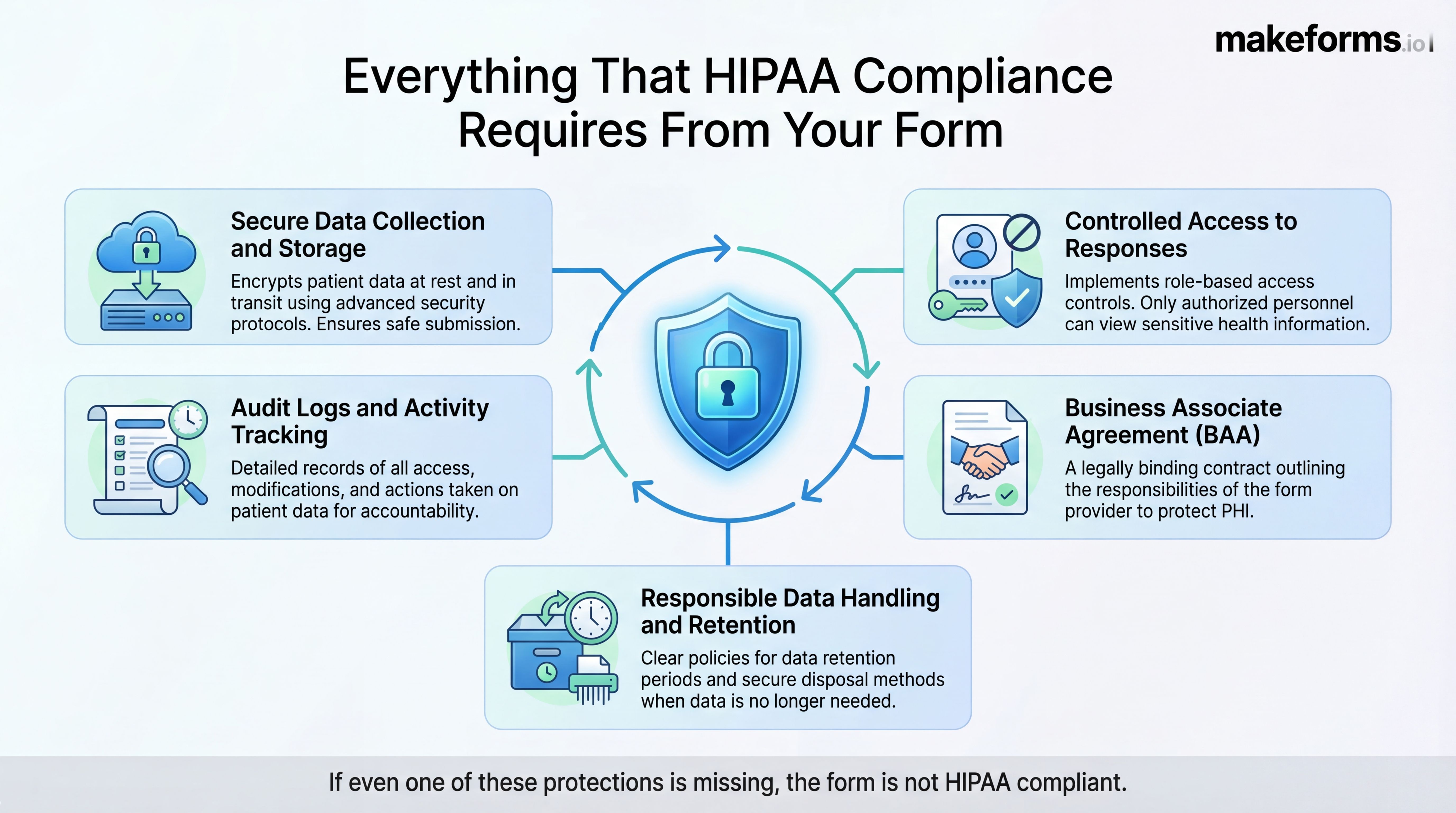
Everything that HIPAA compliance requires from your form
HIPAA compliance isn’t about how a form looks or how many questions it asks. It’s about how patient data is handled after someone clicks submit.
A HIPAA compliant form must protect patient information at every stage. If even one of these protections is missing, the form does not meet HIPAA compliance standards.
Here’s what that protection actually involves.
- Secure data collection and storage - Patient data must be protected during submission and while it’s stored. Information should be encrypted and kept in systems designed for healthcare data, not emailed or stored in plain text.
- Controlled access to responses - Only authorized staff should be able to view or manage patient submissions. Limiting access reduces the risk of accidental or unnecessary exposure.
- Audit logs and activity tracking - HIPAA requires accountability. A compliant form system should record who accessed patient data, when it was accessed, and what actions were taken.
- A Business Associate Agreement (BAA) - If a form provider handles patient data, a BAA is required. Without it, the form is not HIPAA compliant, even if other security measures are in place.
- Responsible data handling and retention - Patient information should be stored only as long as needed and protected from unnecessary access over time. Data shouldn’t be scattered across tools or kept without oversight.
If any of these elements are missing, the form is not HIPAA compliant, regardless of how secure it appears.
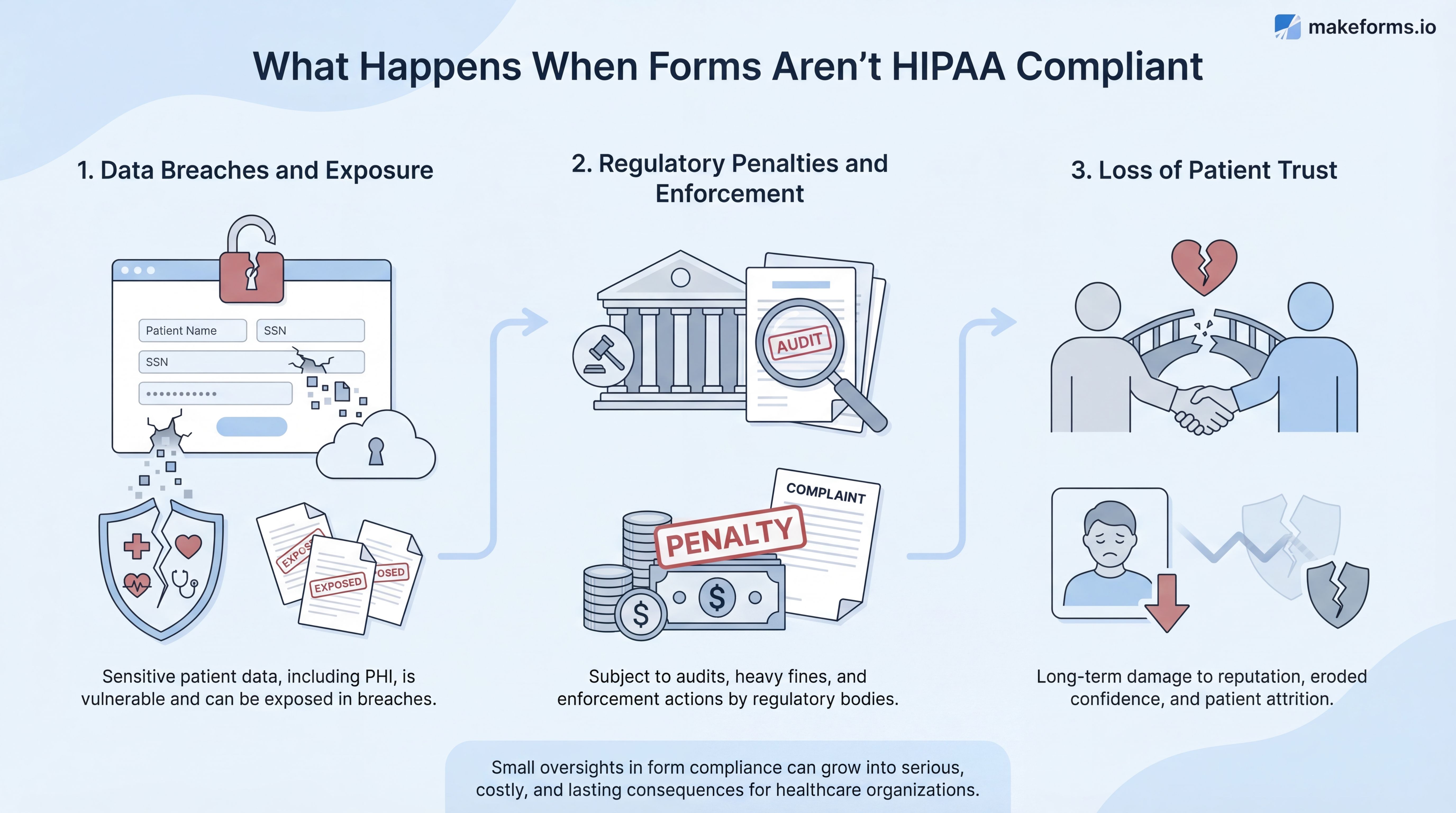
What happens when forms aren’t HIPAA compliant
When forms aren’t HIPAA compliant, the impact isn’t limited to a technical mistake. It can lead to data exposure, regulatory action, and lasting damage to patient trust. These outcomes often start with small oversights, but they don’t stay small.
Data breaches and exposure
Forms that aren’t HIPAA compliant significantly increase the risk of data exposure. This usually isn’t caused by hacking. More often, it comes from how form responses are handled day to day.
Common scenarios include:
- Form responses sent or forwarded through email
- Public or shareable form links without authentication
- Submissions accessible to more staff members than necessary
When protected health information is exposed, it rarely stays an internal issue. HIPAA-related concerns are typically reviewed by the Office for Civil Rights (OCR) within the U.S. Department of Health and Human Services, which investigates complaints, conducts audits, and ensures HIPAA rules are being followed.
Issues may come to light through patient complaints, audits, or when organizations report an incident themselves. In some cases, State Attorneys General may also review violations affecting residents in their state, and in more serious situations involving intentional misuse, the Department of Justice can become involved.
What starts as a form-related data issue can quickly turn into a broader compliance review that requires time, documentation, and corrective action.
Regulatory penalties and enforcement
HIPAA enforcement is based on outcomes, not intent. Even unintentional mistakes can trigger penalties if patient data isn’t adequately protected. What matters is whether reasonable safeguards were in place and whether known risks were addressed.
HIPAA violations fall into two broad categories: civil and criminal, each with different thresholds and consequences.
Civil penalties apply when organizations fail to meet HIPAA requirements due to gaps in processes, safeguards, or oversight. These violations are assessed in tiers based on how preventable the issue was and how the organization responded.
Common civil violation categories include:
- Lack of awareness - The organization did not realize a violation existed but also lacked basic safeguards that should reasonably have been in place.
- Reasonable cause - The issue resulted from misconfigurations, poor access controls, or incomplete compliance measures, such as unsecured forms or shared submission access.
- Willful neglect (corrected) - Known compliance issues were not addressed promptly but were eventually fixed.
- Willful neglect (not corrected) - Known risks were ignored or left unresolved, significantly increasing enforcement severity.
Penalties increase when violations are repeated, affect multiple records, or remain uncorrected.
Criminal penalties apply when HIPAA violations involve knowing or intentional misuse of protected health information. These cases focus on behavior, not configuration errors, and are treated much more seriously than civil violations.
Criminal violations are typically categorized based on intent and impact.
Common criminal violation categories include:
- Knowing unauthorized access - Patient data is accessed without permission, even if no further harm was intended. This includes viewing records without a valid reason or bypassing access controls.
- False pretenses - Patient information is obtained or disclosed under misleading or deceptive circumstances, such as pretending to have authorization when none exists.
- Intent to sell, transfer, or misuse data - Protected health information is used for personal gain, financial benefit, or malicious purposes. This represents the most severe category of HIPAA criminal violations.
Criminal penalties can involve significant fines and, in serious cases, charges against individuals. Unlike civil penalties, which usually apply to organizations, criminal cases can involve employees, contractors, or leaders directly.
These cases are less common, but when they occur, the impact is much more severe and can include long-term legal, financial, and reputational consequences.
Loss of patient trust
Loss of trust is often the most lasting consequence of HIPAA non-compliance.
Patients share health information expecting it to be handled carefully and privately. When that expectation is broken, even unintentionally, confidence drops fast. A single insecure form can make patients question how safely their data is handled across the entire organization.
Unlike technical issues, trust isn’t fixed with a quick update. Patients may hesitate to complete forms, hold back important details, or seek care elsewhere. Over time, this affects engagement, continuity of care, and long-term relationships.
Trust damage also extends beyond patients. Data exposure or compliance reviews can impact an organization’s reputation with partners, insurers, and the wider community.
This is why HIPAA compliance matters at the form level. Forms are often the first point of contact, and when trust breaks there, the impact can last long after the issue is resolved.
Common form mistakes that lead to HIPAA violations
Most HIPAA violations don’t happen because of hacking or bad intent. They happen because forms are set up in ways that don’t account for how healthcare data needs to be handled.
Some of the most common mistakes include:
- Using general-purpose form tools for patient information - Many form builders are designed for surveys or contact forms. When they’re used to collect health information, they often lack the safeguards HIPAA requires, even if the form looks secure.
- Collecting more patient data than necessary - Asking for extra details increases risk. HIPAA encourages collecting only what’s needed for the specific purpose of the form.
- Giving too many people access to form responses - When submissions are visible to entire teams or shared inboxes, patient data is more likely to be accessed by people who don’t need it.
- Saving form submissions on personal devices - Downloading responses to laptops or phones removes important protections and makes data harder to control or track.
- Skipping a Business Associate Agreement with the form provider - If the tool handling patient data isn’t willing to sign a BAA, HIPAA compliance isn’t in place, regardless of other security features.

Each of these choices creates risk on its own. Combined, they are one of the most common reasons forms fall out of HIPAA compliance.
How MakeForms supports HIPAA compliant forms
MakeForms is built to help teams create HIPAA compliant forms without needing legal knowledge or technical setup. Instead of relying on workarounds, compliance is built directly into how forms are created and managed.
Here’s how MakeForms supports HIPAA compliance in practice:
- Encrypted data collection and storage - Patient information is protected during submission and while it’s stored, reducing the risk of interception or exposure.
- Controlled access to form responses - You can decide exactly who on your team can view or manage submissions, so patient data isn’t shared more widely than necessary.
- Audit logs for accountability - Every access and action is recorded, making it easier to track activity and demonstrate HIPAA compliance when needed.
- OTP verification for added protection - OTPs help verify the identity of the person submitting the form, which is especially useful for patient portals, telehealth, and follow-ups.
- Business Associate Agreement (BAA) - MakeForms provides a BAA, ensuring legal accountability for how patient data is handled.
- Response limits and structured data - Submissions stay organized and manageable, helping teams avoid uncontrolled data sprawl.
All of these features work together so compliance is part of the workflow, not something teams have to think about separately.

Creating a HIPAA compliant form with MakeForms
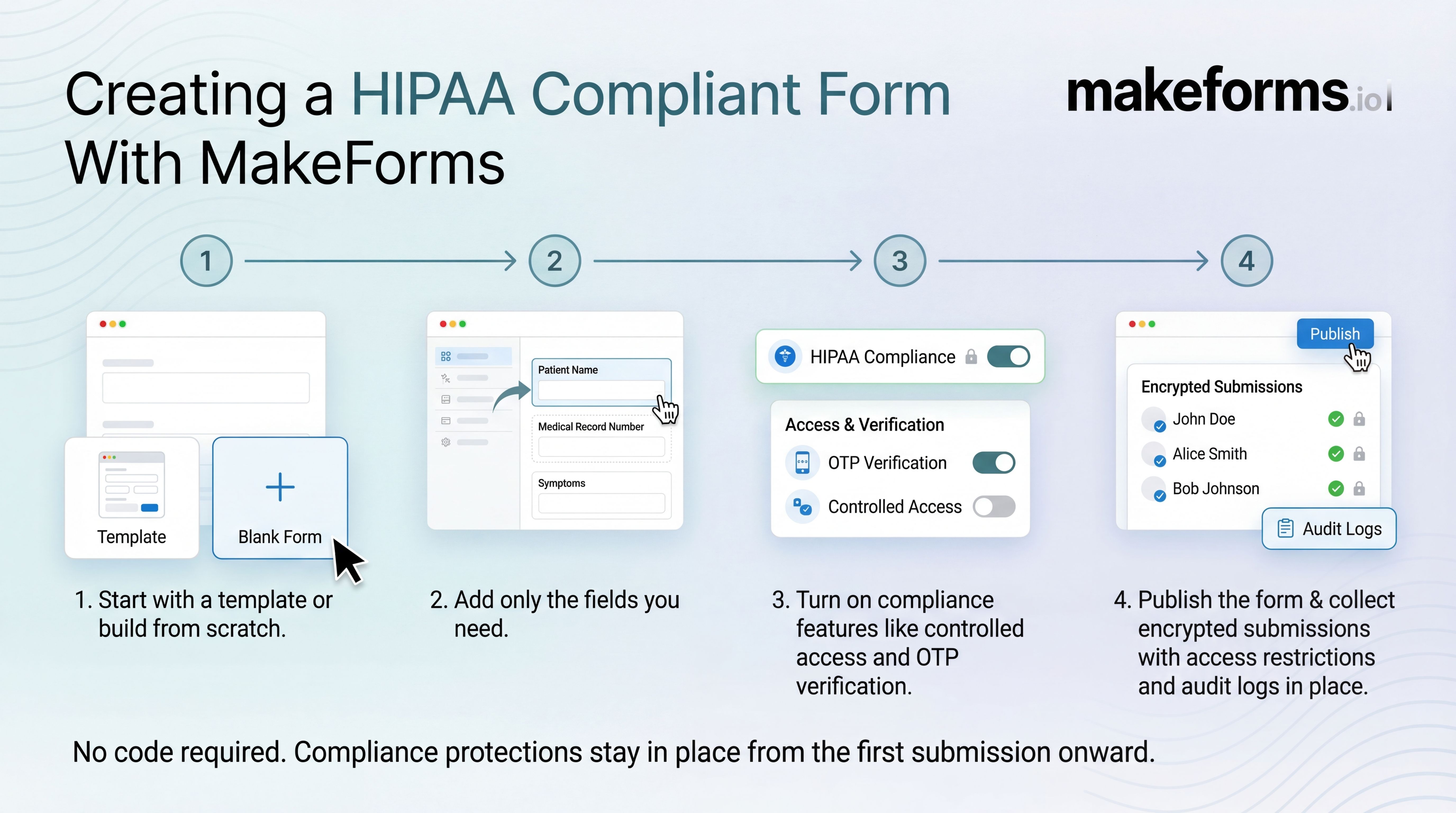
Creating a HIPAA compliant form with MakeForms is designed to be simple, even if you’ve never thought about compliance before.
- You can start with a ready-made template or build a form from scratch, add only the fields you need.
- Turn on compliance features like controlled access and OTP verification.
- Once your form is live, patient data is protected by default.
There’s no code to write and no complex setup to manage. The platform handles the technical and compliance requirements behind the scenes.
Submissions are encrypted, access is restricted, and activity is logged automatically. As your workflows change or your team grows, those safeguards stay in place without extra effort.
This means healthcare teams can collect patient information with confidence, knowing their forms meet HIPAA requirements from the first submission onward, while staying focused on patient care and daily operations rather than compliance maintenance.
Build your first HIPAA compliant form with MakeForms. No code required.